TEE Fusion Imaging Brings Precision View to TMVR
Case study demonstrates capability of 3D image overlay to precisely pinpoint and address mitral paravalvular leak
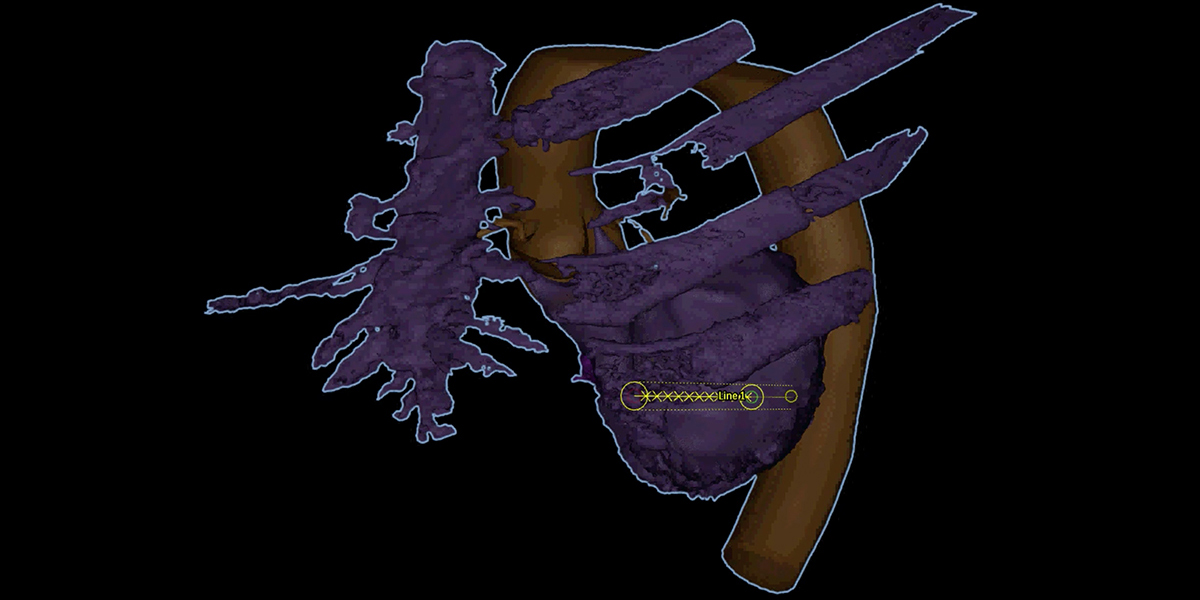
TEE fusion imaging capability at Hackensack Meridian Hackensack University Medical Center allows more precision valve procedures to take place in the cath lab versus surgery. A recent case featuring TEE-guided combined mitral paravalvular leak closure and ViV TMVR demonstrates this capability.
The patient, a 73-year-old male with a history of HTN, HLD, CHF and atrial fibrillation, presented with acute chronic heart failure. He had a history of aortic and mitral valve endocarditis and underwent successful surgical bioprosthetic combined valve replacement in 2017.
The patient was doing well until recently when he developed shortness of breath. Physicians ultimately determined his symptoms were due to a leakage near the mitral valve perimeter, known as a paravalvular leak (PVL). When a large PVL forms in the tissue surrounding a surgically implanted valve, the treatment requires closure of the hole causing the leak.
Traditionally, this would involve a repeat open heart heart surgery, which would be a high risk procedure. Recent advances allow specially trained interventional cardiologists to place closure devices in this hole using catheters to stop the leak and prevent the patient from requiring another operation. However, depending on the exact location, precisely advancing wires through a catheter to the exact location can be challenging with 2D imaging alone.
At Hackensack University Medical Center, the use of real-time 3D image modeling improves planning and execution of PVL closure procedures. Before the procedure, imagers model the chambers of the heart and the valve location based on a pre-procedure CT scan. This 3D view is then overlaid onto the real-time echocardiographic and fluoroscopic imaging during the procedure, modeling the precise location of the valve pathology. This allows far greater accuracy in pinpointing locations within heart anatomy and catheter location.
“Throughout the procedure, we are able to visualize the heart chambers, prior surgical valve and PVL using 3D imaging in real time by combining three differrent imaging modalities to generate a 3D model of the heart in real time. These images improve the accuracy of device deployment and shorten procedure times. Ultimately, this results in safer and more reliable outcomes,” said Ryan Kaple, M.D., FACC, FSCAI, director of the Structural and Congenital Heart Program, Hackensack University Medical Center.
Creating the TEE Fusion image guidance requires a team effort, and coordination with imagers, surgeons and heart failure specialists. TEE and cardiac CT are fundamental in planning this procedure, evaluating the PVL size and locations, and differentiating between valvular and paravalvular regurgitation, and ruling out valvular dehiscence.
In this mitral paravalvular leak case, the structural interventional cardiologist, Tilak Pasala, M.D., worked with the imaging team to perform this complex procedure. Dr. Pasala identified two leaks around the surgical mitral valve. Both leaks were crossed with a soft guidewire after obtaining transseptal access through a vein in the leg. Both PVLs were plugged with specialized closure plugs. Next, the degenerated surgical mitral valve was addressed. Going through the vein in the leg, a new bioprosthetic valve was implanted within the prior surgical mitral valve. The mitral ViV deployment followed, and final imaging confirmed a fully opening VIV mitral prosthesis and location of the 2 PVL plugs.
With the catheter-based therapies such as mitral ViV and PVL closure, patients can now often avoid repeat open heart surgery. When evaluating surgery on a potentially frail patient with heart failure, a repeat open heart surgery is often high risk.
Hackensack University Medical Center averages 400 transcatheter valve procedures annually and employs TEE Fusion 3D imaging in nearly all. The center’s core imaging lab, a recognized center of excellence in cardiac imaging, draws large-scale device clinical trials to select Hackensack University Medical Center to conduct participating patient imaging.
Learn more about innovative cardiovascular care at Hackensack University Medical Center.
