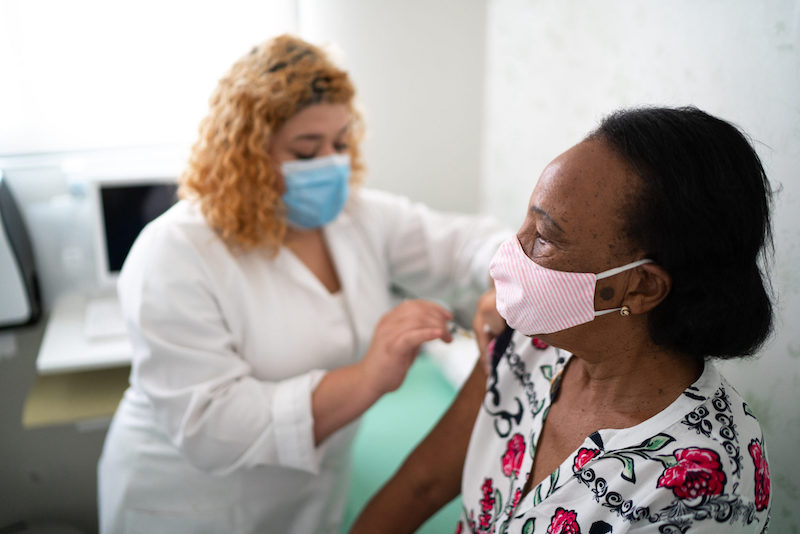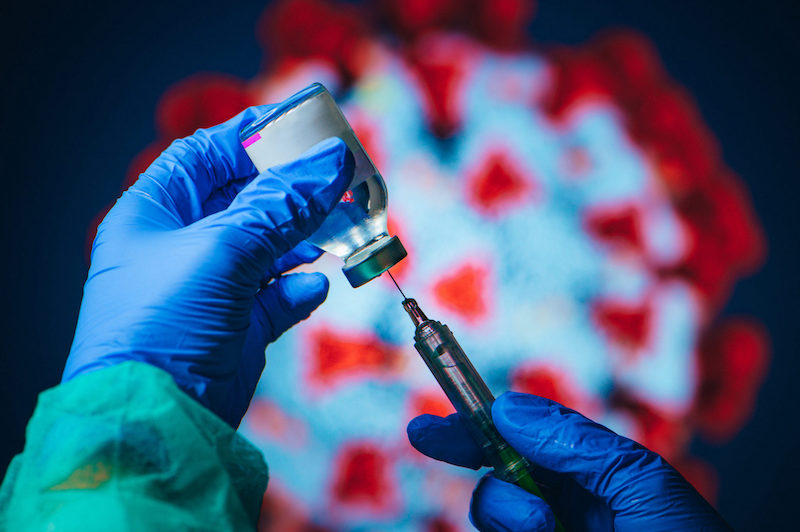
The United States has begun to roll out COVID-19 vaccines in an effort to help stop the pandemic. Millions of people, beginning with health care workers, will line up across the country to get the vaccine.
For many, we’ve never really thought about the approval process that every vaccine, including the COVID-19 vaccine, must go through before getting approved for public use. It’s an extensive and rigorous process to ensure it’s safe before it can be distributed to the community.
However, with the COVID-19 vaccine being developed at record-breaking speed it’s normal to question the process. That’s why we talked to Ihor Sawczuk, M.D., chief research officer at Hackensack Meridian Health about the federal approval process for vaccines as well as why these new COVID-19 vaccines are safe for most people.
Fast Facts
“It’s important to know that while these vaccines are being developed in record time, we’re still doing all three phases of clinical trials, and all of the same steps are being taken to look at the data out of these clinical trials to help determine if each of these vaccines are approved,” says Dr. Sawczuk. Here are a few quick facts to get you up to speed on the vaccines:
- Thousands of people have already voluntarily tested several vaccines in clinical trials to ensure it’s safe
- The data from those trials has been studied by career scientists at the Food and Drug Administration (FDA) as well as a separate and independent advisory committee of medical and public health experts
- The FDA will only grant emergency use authorization to each vaccine once it has determined that it is safe and effective. FDA scientists also look to ensure that the benefits of the vaccine outweigh the risks.
- Vaccines produced at scale are made in batches called lots. Each of those lots are tested for safety and potency.
- Record amounts of public funding are being poured into the developments of these vaccines, helping power the accelerated timeline.
- Many prominent and public figures in health and government have signaled that they will take the vaccine when it becomes available, including former Presidents Bill Clinton, George W. Bush and Barack Obama as well as national vaccine expert Dr. Anthony Fauci and others.
Vaccine Development Timeline
While the development of the COVID-19 vaccine happened at a record pace, no scientific or safety evaluations were skipped over. Rigorous clinical trials took place with tens of thousands of participants to ensure safety and efficacy. Additionally, the government prepurchased vaccines and began manufacturing them before they were approved, ensuring a swift distribution process once the Food and Drug Administration (FDA) and the Centers for Disease Control and Prevention (CDC) finished their rigorous evaluations of each vaccine.

How Clinical Trials Work
Before a new vaccine is ever given to the public, it must undergo a clinical trial to determine:
- Is the vaccine effective at treating the illness?
- Does the vaccine produce any harmful side effects?
- Do the vaccine’s benefits outweigh any risks involved?
This process is completed in three phases. During this process, vaccines are tested on human volunteers. The FDA sets the rules for these three phases to ensure the safety of the volunteers. Learn more about the steps researchers take to ensure clinical trials are safe.
Phase 1
Phase 1 trials usually involve between 20 and 100 healthy volunteers. They are given the vaccine and monitored closely. In this phase of the trial, researchers are working to determine:
- Is this vaccine safe?
- Does this vaccine seem to work?
- Are there any serious side effects?
- What is the safe effective dose?
Phase 2
Phase 2 clinical trials typically enroll volunteers numbering into the hundreds. Again, they are given the vaccine and monitored closely. Here, researchers hope to understand:
- Is this vaccine safe?
- How do each of the volunteers’ immune systems respond to the vaccine?
- What are the common short-term side effects?
Phase 3
In Phase 3 clinical trials, research teams give the vaccine to thousands of volunteers. By giving the vaccine to such large numbers of people, researchers are looking to answer:
- Is this vaccine safe?
- How do people who get the vaccine compare to people who did not (placebo)?
- Is the vaccine effective?
- What are the most common side effects in most people?
Regulatory Review and Approval
Once clinical trials are complete the vaccine developers compile all the data from phases 1, 2 and 3, and share it with the FDA and the Advisory Committee on Immunization Practices (ACIP) COVID-19 Work Group, a collaboration of medical and public health experts from across the country.
These groups will study the data and use a framework to determine if they can recommend that the vaccine is safe and effective. Key factors considered in development of recommendations include:
- balance of benefits and harms
- type or quality of evidence
- values and preferences of the people affected
- health economic analyses
Emergency Use Authorization (EUA)
At this point a vaccine developer may apply for what’s known as an emergency use authorization (EUA).
An EUA is used during an emergency such as the COVID-19 pandemic to help make certain products available that have been found to diagnose, treat, or prevent serious or life-threatening diseases. Standard for an EUA is the product “might be effective.” EUA’s have historically been used to allow deployment of a medical countermeasure when known potential benefits outweigh known potential risks.
However, it’s important to note that the risk and benefit analysis can vary across populations and demographics.
Biologic License Application (BLA)
A biologic license application is approved only if FDA determines there is substantial evidence of safety and effectiveness from adequate, controlled trials.
While some upcoming COVID-19 vaccines may receive an EUA, the FDA has signaled that it will utilize standards that more closely resemble a BLA. Guidance released in October showed that the FDA would require two months of follow-up after a patients’ second vaccination prior to EUA approval.
Manufacturing
A critical aspect to a mass vaccine program is ensuring that there are enough vaccines for everyone in the population.
Vaccine manufacturers commonly begin large-scale production of COVID-19 vaccine candidates during Phase 2/3 trials to ensure there’s enough of the vaccine available right away if it’s found to be safe and effective. If a vaccine candidate is found to be ineffective or unsafe, the manufacturer would destroy those doses.
During the manufacturing process, vaccines are produced in batches called lots. These lots are tracked and tested individually to ensure they are safe and potent. Lots can only be released once the FDA reviews their safety and quality.
Tracking Side Effects
Even after a vaccine is granted an authorization or license to being distribution to the public, federal regulators from the FDA and CDC will continue to monitor for adverse events or possible side effects with the drug.
The Vaccine Adverse Event Reporting System (VAERS) was designed to collect and analyze public reports of adverse events that happen after receiving a vaccine. Anyone can submit a report to this system including patients, parents or caregivers and even health care professionals.
V-SAFE, is a new smartphone after-vaccination health checker app for people who receive COVID-19 vaccines. V-SAFE will use text messaging and web surveys from CDC to check in with vaccine recipients for health problems following COVID-19 vaccination. The system also will provide telephone follow up to anyone who reports significant adverse events.
You should always contact your health care provider first if you think you are experiencing a side effect after receiving any vaccination.
Next Steps & Resources:
- Meet our clinical contributor: Ihor Sawczuk, M.D.
- To make an appointment with a doctor near you, call 800-822-8905 or visit our website.
Sources:
Find a doctor near me

COVID-19 Vaccine Trials: 9 Things You Should Know

How to Prepare for Your COVID-19 Vaccine

COVID Vaccine and Children: What to Know