All About the mRNA COVID-19 Vaccine and Allergies
January 11, 2021
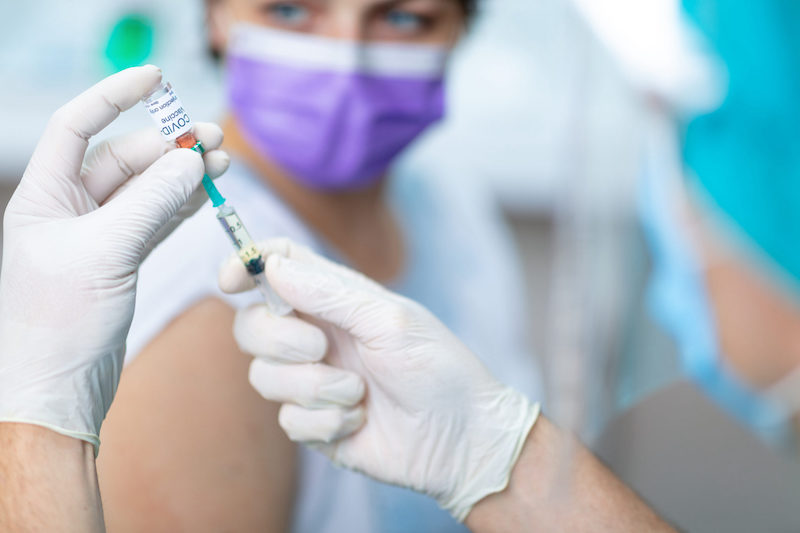
The vaccine for COVID-19 is here and being distributed to millions across the country. With this development, there have been a few reports of some individuals experiencing allergic reaction to the vaccine.
While only one person who received the vaccine in clinical trials experienced a severe allergic reaction (anaphylaxis), once widespread vaccination of health care works started in the United Kingdom and United States, a few reports of presumed severe allergic reactions to the vaccine prompted the Centers for Disease Control and Prevention (CDC) to issue an updated recommendation for those with a history of allergies. We’ve talked to Juan Ravell, M.D., division chief of allergy and immunology at Hackensack University Medical Center to get some clarity around who should stay away from the vaccine, different types of allergies and how they associate with the vaccine and when you should be concerned about an adverse reaction.
Who should not get the mRNA COVID-19 vaccine?
While both the Pfizer-BioNTech and Moderna mRNA COVID-19 vaccines have been deemed safe and effective at preventing symptomatic COVID-19 infection, some people should consult their allergist or immunologist before getting the vaccine.
- The mRNA COVID-19 vaccine should not be administered to individuals who have had a severe allergic reaction to any component of the Pfizer-BioNTech or Moderna mRNA COVID-19 vaccines. Although the specific component responsible for the severe allergic reactions has not been identified, anaphylactic reactions to polyethylene glycol, a component in the COVID-19 vaccine, have been rarely reported. PEG is an ingredient in some other vaccines and multiple FDA-approved medications, including bowel preparations, Miralax and Depomedrol.
- At the time of this writing, children and adolescents under the age of 16 and 18 years for the Pfizer-BioNtech and Morena vaccines, respectively, should not receive the mRNA COVID-19 vaccine. This recommendation may change once clinical trials are conducted in children.
The following persons should be evaluated by an allergist/immunologist to determine whether they can safely receive the vaccine:
- Individuals with immediate allergic reaction of any severity to a previous dose of an mRNA COVID19 vaccine or any of its components.
- Individuals with immediate allergic reactions of any severity to polysorbate. This recommendation is based on the potential allergic cross-reactivity with the vaccine component PEG.
- Individuals who have previously had a severe allergic reaction to any vaccine or injectable therapy (i.e. intravenous, intramuscular or subcutaneous therapies)
- Individuals with a history of anaphylaxis of unknown case (idiopathic anaphylaxis).
The mRNA COVID-19 vaccine should not be simultaneously administered with other vaccines. The CDC recommends a minimum interval of 14 days before or after administration of any other vaccine. The mRNA COVID-19 vaccines can be administered to immunocompromised patients though its efficacy may depend on their underlying immune defect.
These recommendations only apply to the current mRNA COVID-19 vaccines and may change over time as new data become available.
What if I have other types of allergies like seasonal, food or pet?
The CDC considers any history of allergies as a precaution, but not a reason to avoid getting the vaccine. Individuals with allergies to medications, foods, environmental allergens, insects and latex have the same risk of having an allergic reaction to the mRNA COVID-19 vaccines as the general population.
When you get your vaccine, the site will monitor you for 15 minutes (30 minutes if you have a history of allergies) to ensure that any adverse reaction can be identified and addressed promptly.
Be sure to talk to the provider administering your vaccine about any concerns you may have with allergies prior to receiving the injection.
How do I know if I’m having an allergic reaction to the vaccine?
Anaphylaxis is an acute, severe and potentially life-threatening allergic reaction and can occur rarely after vaccination. Early recognition of signs and symptoms of anaphylaxis is extremely important because an anaphylactic reaction can progress quickly. Therefore, people who receive the Covid19 vaccine should be monitored for 15-30 minutes after getting the injection to ensure that allergic reactions are promptly recognized and treated according to their severity. The cause of anaphylaxis is usually contact with an allergen (usually a protein) to which a person’s immune system has become sensitive. The clinical presentation of anaphylaxis can vary from person to person, but the most common symptoms include:
- Cutaneous symptoms such as hives (urticaria) and swelling of the skin (angioedema). Itching and flushing are also common.
- Respiratory symptoms are common, especially in individuals with asthma or other underlying lung diseases. These include shortness of breath, chest tightness, wheezing, and coughing.
- Throat closing sensation, stridor (high-pitched sound while breathing).
- Gastrointestinal symptoms such as nausea, vomiting, diarrhea, abdominal pain.
- Cardiovascular symptoms, including dizziness, fainting, fast heart rate, low blood pressure.
- Neurological symptoms: anxiety, confusion, sense of impending doom.
Mild allergic reactions may not require administration of an EpiPen and can be managed with antihistamines.
The provider administering your vaccine will monitor you for these symptoms and should be well-equipped to handle any emergency that may arise.
Next Steps & Resources:
- Meet our clinical contributor: Juan Ravell, M.D., division chief of allergy and immunology at Hackensack University Medical Center
- Hackensack Meridian Health – Vaccine Updates
- Need a doctor near you? Call 800-822-8905 or visit our website.
The material provided through HealthU is intended to be used as general information only and should not replace the advice of your physician. Always consult your physician for individual care.
Behind the COVID-19 Vaccine Approval Process
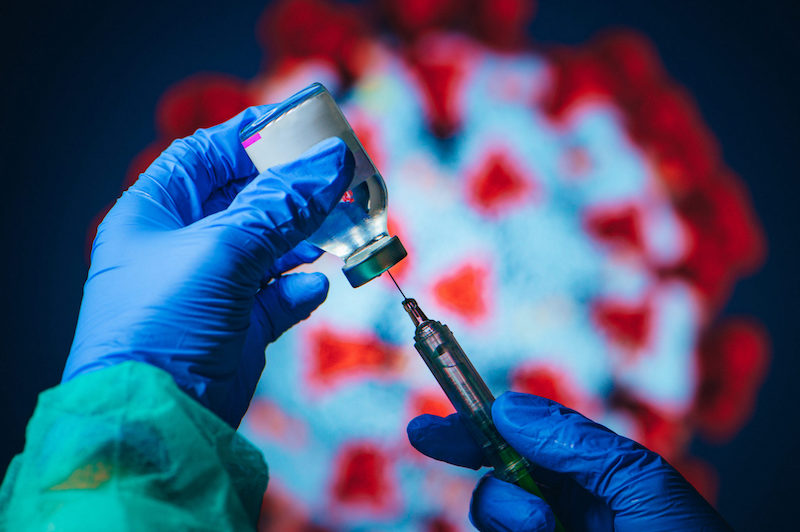
The United States has begun to roll out COVID-19 vaccines in an effort to help stop the pandemic. Millions of people, beginning with health care workers, will line up across the country to get the vac...
A Simple Breakdown of the Ingredients in the COVID Vaccines

If you’re among the many wondering “what’s actually in it?” and, “is it safe to receive the injection?”, read on.
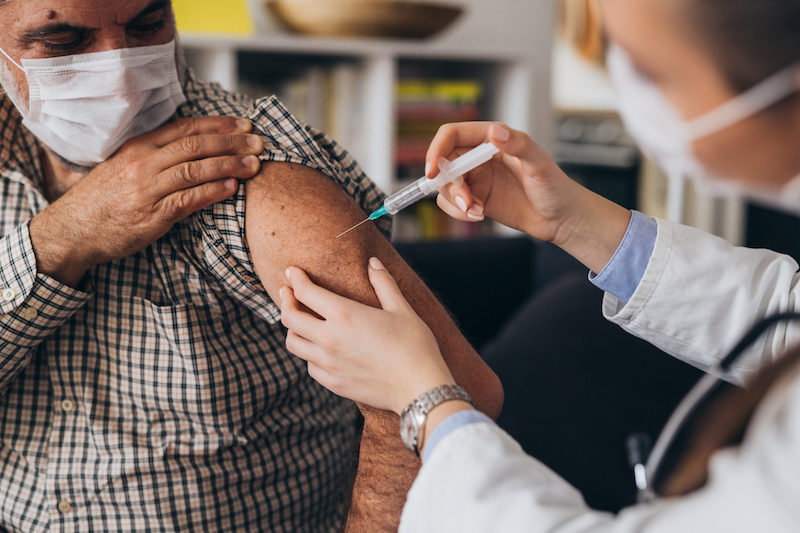
Recovered from COVID-19? Why You Still Need a Vaccine
Dr. Thomas Bader has answered common questions about the COVID-19 vaccine that you may have if you’ve already experienced the illness
What Can You Do After You’re Fully Vaccinated Against COVID?
There are advantages to getting fully vaccinated against COVID-19.
Can You Get COVID-19 Twice?
Some diseases, like measles, can only infect us once. What about COVID-19?
What Are COVID-19 Vaccine Side Effects, and How Long Do They Last?
Here are answers to questions that you may have about COVID-19 vaccine side effects.