Hepatobiliary and Pancreatic Cancer Care in New Jersey
At Hackensack Meridian John Theurer Cancer Center, our dedicated team provides comprehensive, patient-centered care using the most advanced treatments available. We are here to guide you through every step of your journey, from diagnosis to recovery.
About Hepatobiliary and Pancreatic Cancer
Hepatobiliary and pancreatic cancers are complex diseases that affect vital organs in the abdomen. Because these organs are located close together and are functionally related, they are often managed by the same team of specialists.
What is Pancreatic Cancer?
The pancreas is a gland located deep within the abdomen, positioned between the stomach and the spine. It plays two critical roles: producing enzymes for digestion and releasing hormones like insulin to regulate blood sugar.
Pancreatic cancer develops when cells in the pancreas begin to grow and divide uncontrollably. Normally, your body creates new cells only when needed. When this process breaks down, a mass of excess tissue, known as a tumor, can form. These tumors can disrupt the pancreas's vital functions and may spread (metastasize) to other parts of the body, such as the liver, lungs, bones, or lymph nodes.
Types of Pancreatic Tumors
Pancreatic tumors are broadly classified based on the type of cell they originate from:
- Exocrine Tumors: These are the most common type. Adenocarcinoma, which begins in the cells lining the pancreatic ducts, accounts for over 90% of all pancreatic cancer diagnoses.
- Neuroendocrine Tumors (PNETs): A rarer type of tumor that forms in the hormone-producing islet cells of the pancreas.
What are Hepatobiliary Cancers?
The term "hepatobiliary" refers to the liver, bile ducts, and gallbladder. Cancers in this system are closely linked to pancreatic cancer due to their proximity and shared ductal systems. An integrated approach is essential for effective treatment.
Diagnosis and Advanced Treatment at John Theurer Cancer Center
Accurate diagnosis is the first step toward creating an effective treatment plan. Our team uses state-of-the-art imaging and diagnostic tools to determine the exact type, stage, and location of your cancer.
At the John Theurer Cancer Center, we believe in a multidisciplinary, integrated approach to cancer care. Our specialists collaborate to curate a personalized treatment plan tailored to your specific needs.
Why Choose Us for Your Cancer Care?
As a designated National Pancreas Foundation (NPF) Center of Excellence, we are recognized for providing the highest level of expert care. This designation gives us the resources and expertise to offer you the most effective treatment for your specific type of hepatobiliary or pancreatic cancer.
Our comprehensive treatment options include:
- Robotic and Minimally Invasive Surgery: Utilizing state-of-the-art technology to precisely remove tumors, leading to faster recovery times, less pain, and minimal scarring.
- Advanced Medical Therapies: Access to the latest in chemotherapy, targeted therapy, and immunotherapy designed to fight cancer at a cellular level.
- Formal Pancreas Cancer Screening Program: We offer a dedicated screening program for high-risk individuals, focusing on early detection when cancer is most treatable.
Screening and Diagnosis
Treatment Options
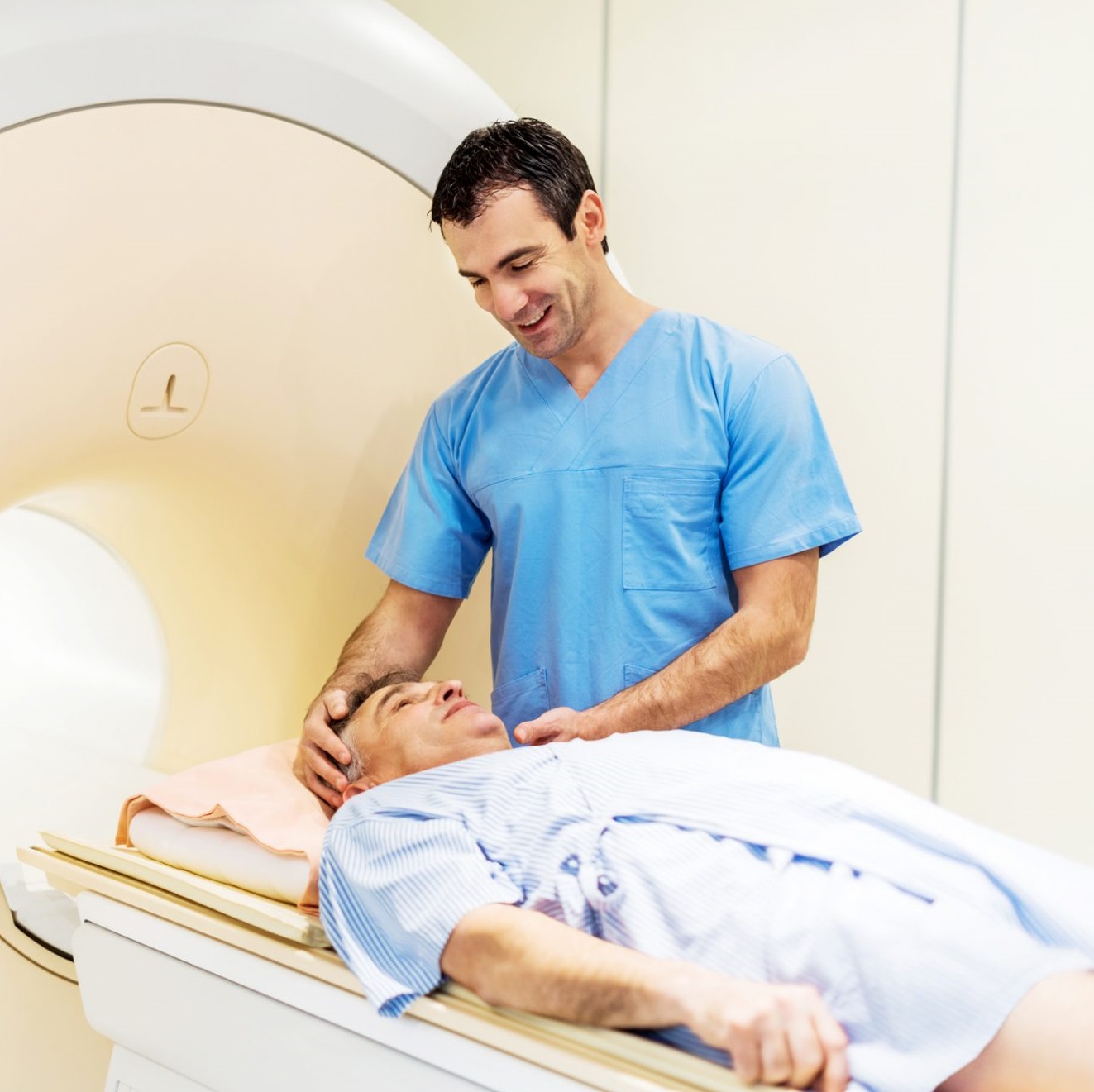
What to Expect From Radiation Therapy
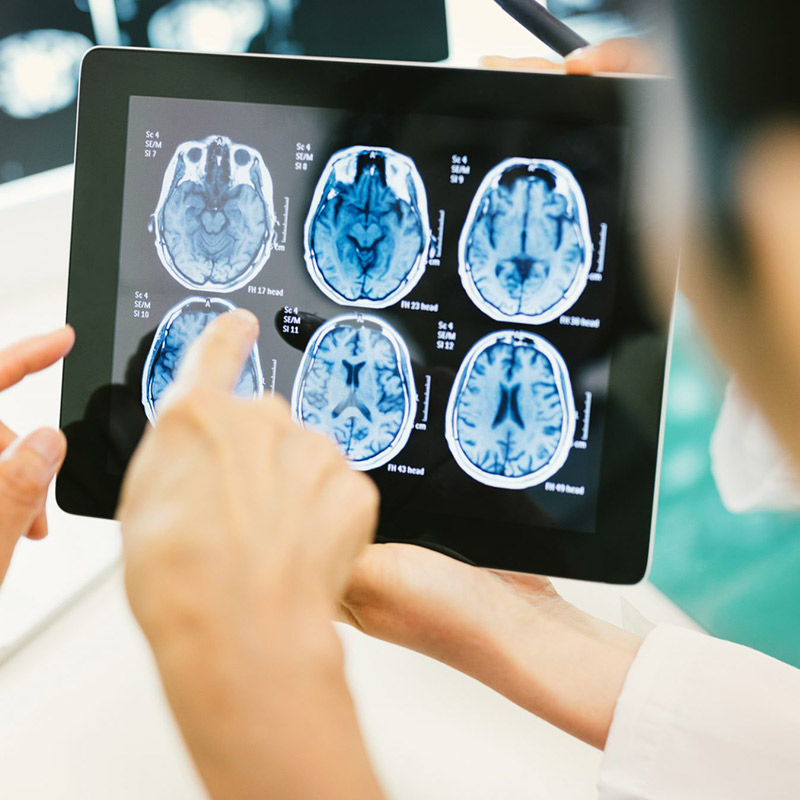
What Are the Early Symptoms of a Brain Tumor?
Manage Living with Chronic Illness