Gastroenterology at Hackensack
Meridian Health
Meridian Health


A colonoscopy is a simple outpatient exam that helps uncover any potential digestive issues, such as Colitis, Diverticulosis and colon cancer.
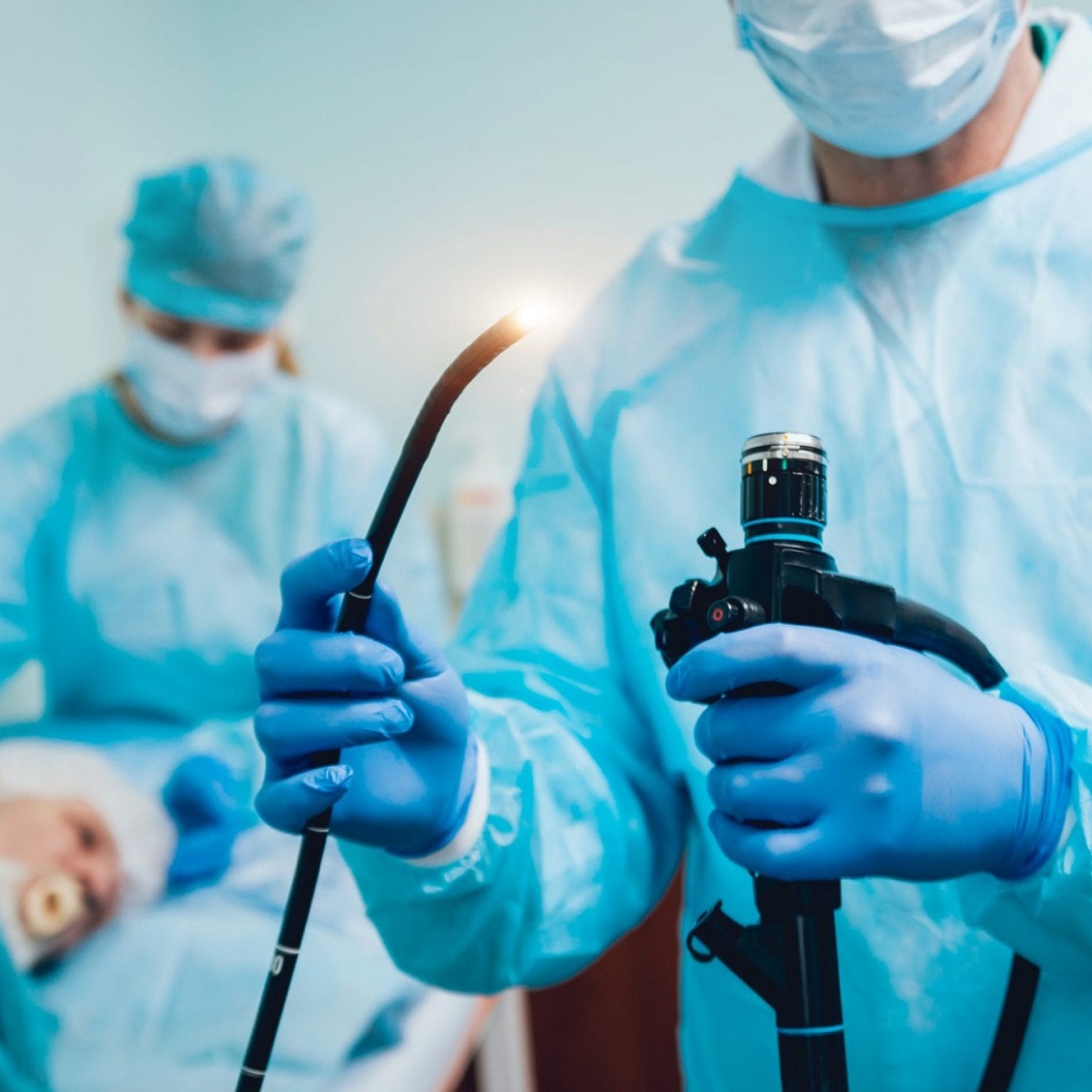
A colonoscopy visually examines your entire colon using a long flexible tube with a small camera at the end. During the procedure, a video monitor in the exam room shows the images captured on camera. The physician watches the monitor and may also remove tissue samples (biopsies) or polyps for further tests.
Take Our Free Colon Health Assessment
Find a gastroenterologist, colonoscopy procedure location, learn more about why you should choose Hackensack Meridian Health, or view all of our gastrointestinal services and the conditions we treat.
To allow for a thorough exam, your lower colon should be clean. This means you may only drink clear liquids, along with taking laxatives or an enema the day before the procedure.
Bloating and bowel distension are common and should only last about 30 to 60 minutes after the procedure. If your physician removes biopsies or polyps during the exam, you may experience some spotting of blood afterward. However, this is rarely serious. You should not drive or operate machinery for the remainder of the exam day.
Your physician will be able to provide you with additional information before your exam day.
How to Prepare for a ColonoscopyYou may be due for a colonoscopy if any of the following apply:
A colonoscopy is a preventative measure to help detect potential issues at an early stage, even before you may experience any symptoms.
It is also helpful in allowing your physician to diagnose the cause of certain symptoms you may already be experiencing, such as:
Endoscopists can find and treat problems during the procedure. They commonly remove any polyps (abnormal growths) that they find and can test them for cancer. The removal of polyps also prevents possible cancer from developing or spreading.
During your colonoscopy, the endoscopist can:
If a polyp or cancer is detected, our team of colorectal cancer specialists provide the most advanced approaches – including advanced endoscopic or robotic surgery and clinical trials of the latest treatments. Our goal is to cure your colorectal cancer and minimize side effects to help you maintain an optimal quality of life. Other type of exams include barium X-rays and stool samples. Your physician will discuss which type of exam is best for you. Learn more about your treatment options.
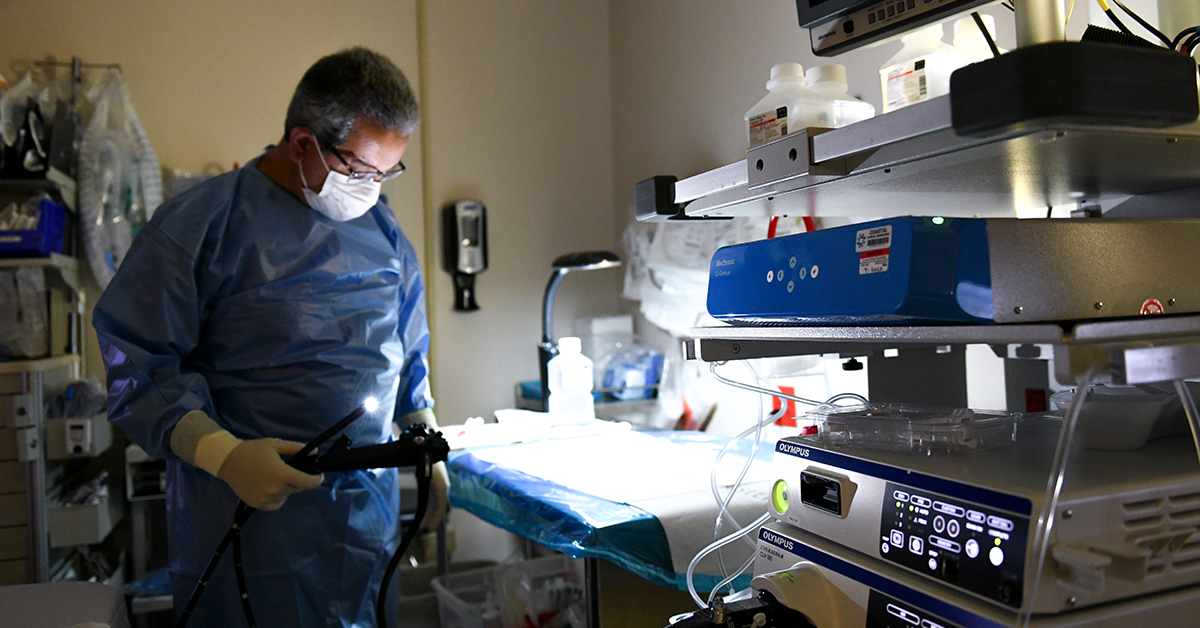
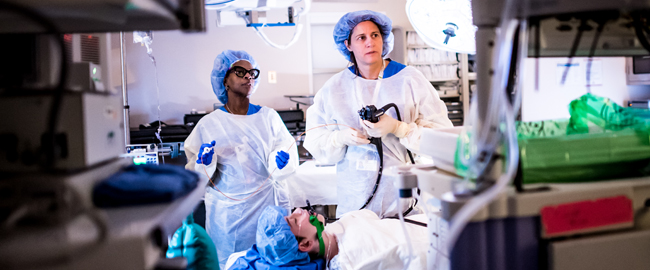
Hackensack University Medical Center is the only hospital in New Jersey, and the first in the tri-state area, to receive a grant to provide artificial intelligence (AI) assisted colonoscopy technology to low-income and underserved communities. The AI endoscopy module, authorized by the FDA in April 2021 uses computer-aided detection algorithms to identify colorectal polyps of varying shapes and sizes in real time, facilitating the diagnosis and prevention of colorectal cancer, the second leading cause of cancer-related death in the U.S. At the discretion of their doctor, any patient having a screening colonoscopy can be screened with the assistance of AI at no extra cost and the procedure is covered by all insurances. Patients with a history of polyps; younger patients and patients with a history of inflammatory bowel disease are likely to benefit most from the increased precision of the test.