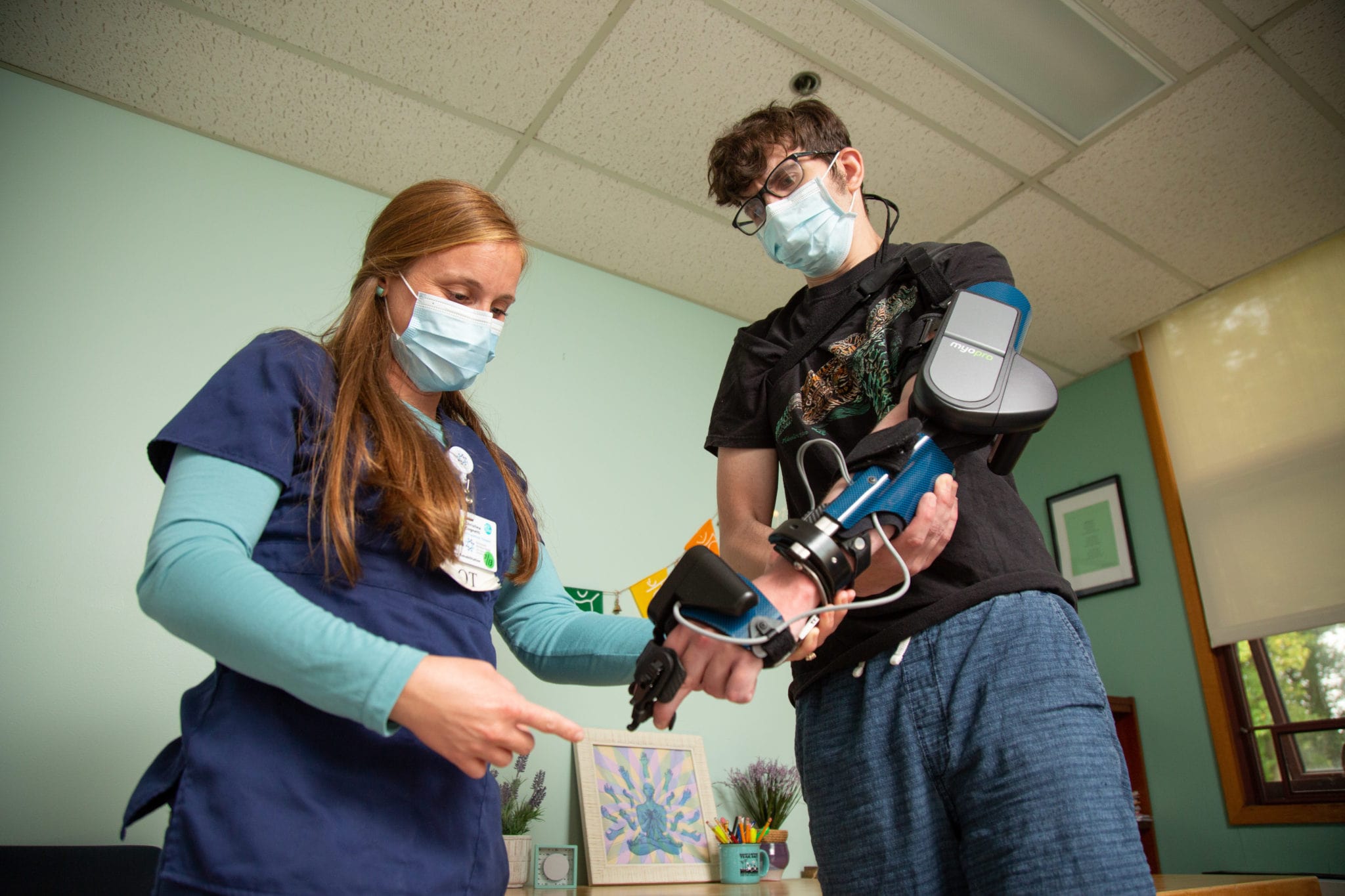
Each year in the U.S., more than 795,000 people have a stroke. But many people don’t realize that 25 percent of people who have a stroke will go on to have a second stroke.
According to Sara Cuccurullo, M.D., medical director and vice president of JFK Johnson Rehabilitation Institute and Talya Fleming, M.D., medical director of the Stroke Recovery & Aftercare Program at JFK Johnson Rehabilitation Institute, here are a few steps that stroke survivors can take to lower their risk of a second stroke:
- Quit smoking.
Smoking is one of the leading causes of cardiovascular (heart) disease and stroke. Quitting smoking can reduce the risk of having a second stroke by two to four times. And even if you have been smoking for a long time, it’s never too late to benefit from quitting.
- Optimize medications and manage chronic conditions.
For people who have been diagnosed with chronic disease — including atrial fibrillation (irregular heartbeat), high blood pressure, diabetes and high cholesterol — taking medications is critical for controlling the condition and preventing stroke.
- Manage diet and weight.
“Research shows that patients who adopt a Mediterranean diet — which is rich in vegetables, fruits, whole grains, healthy fats, poultry, fish, beans and eggs — reduce their risk of coronary heart disease and stroke risk by 20 percent,” says Dr. Cuccurullo.
Adopting a healthy diet also goes a long way toward helping to maintain a healthy weight. If you are overweight or obese, losing 5-10 percent of your body weight can significantly reduce your stroke risk.
- Increase cardiovascular activity.
Increased cardiovascular activity plays a huge role in improving function, reducing mortality and preventing a second stroke.
“Our Stroke Recovery Program includes 36 sessions of monitored cardiovascular exercise, similar to cardiac rehabilitation,” says Dr. Fleming, who said the program uses recumbent bikes to help stroke survivors safely increase activity levels.
Dr. Fleming says that patients who participated in the program also had a 103 percent increase in cardiovascular function and a 22 percent reduction in hospital readmissions within one year for all causes.
- Seek support.
Dr. Cuccurullo and Dr. Fleming agree that post-stroke care provided by rehabilitation experts, combined with a robust family support system, contributes to improved outcomes for stroke survivors.
“Our patients do better, get better faster and function better,” shares Dr. Cuccurullo. “Stroke recovery is also linked to improved self-care and quality of life, which is tied to a lower risk of depression.”
“Our program can be the difference between going home after a stroke and requiring full-time in-home or facility-based care,” adds Dr. Fleming.
When to Seek Medical Care
Because people who have already had one stroke are more likely to have another, it’s essential to recognize the warning signs and seek immediate care. To help you identify the signs and symptoms of stroke, remember “BE FAST”:
B – Balance difficulties
E – Eyesight changes
F – Face weakness
A – Arm weakness
S – Speech difficulties
T – Time to call 911
And while it’s true that getting immediate stroke care can improve survival rates and overall outcomes, individuals and families also need to know where to turn for post-stroke care.
“Our comprehensive program incorporates rehabilitation, cardiovascular conditioning, nutritional education, psychology, risk factor assessment and follow-up visits to check on progress,” shares Dr. Fleming. “Our research shows that people who participate in a comprehensive stroke rehabilitation program have significantly improved overall outcomes including decreased mortality, decreased readmissions, increased cardiac capacity and improvement in function.”
Find a doctor near me

Tinnitus Patient Finally Finds Peace and Quiet

Which Screening Technology Is Right for Me?
Five Tips for a Healthier Workout