
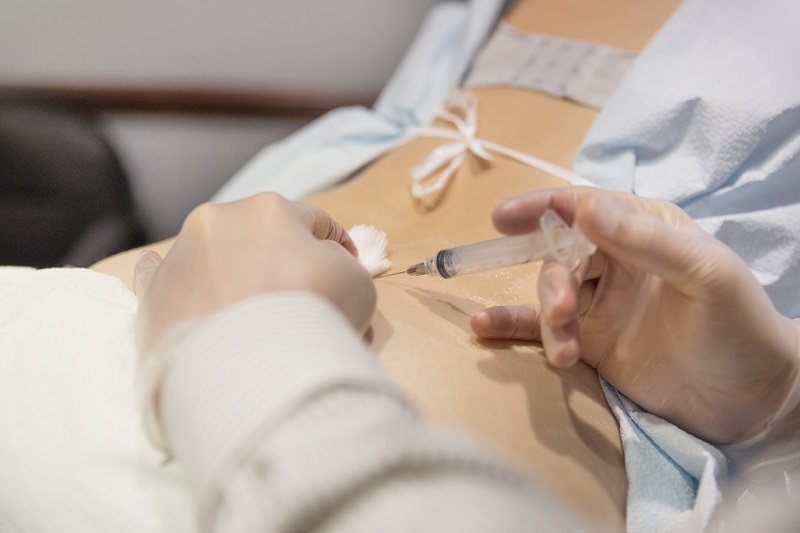
You’ve tried physical therapy, medications and other non-invasive options, and yet, your back still hurts. Enter - back pain injections.
Epidural steroid injections (ESIs) are a type of spinal injections that use a combination of numbing medication, steroids and saline to help alleviate pain in the back and legs associated with common spinal conditions.
Pain management expert, Mike Mizrahi, D.O. explains what you can expect during an injection for back pain, who’s a good candidate for this type of procedure and how long relief can last.
What to Expect During an Injection for Back Pain
- Check-in for your appointment.
You’ll be welcomed at the front desk, asked to provide your license and insurance card, and then sign a few forms. Once the team is ready for you, they will bring you into a pre-procedure patient room or waiting area.
-
Change into a gown (opening to the back) and have your vital signs taken.
You will have your weight and temperature taken, and your heart rate, blood pressure and oxygen saturation will be monitored. If you are diabetic, a blood glucose test may also be taken. For those who could be pregnant, a urine pregnancy test will be taken. Your allergies and current medications will be verified.
It’s best if you wear comfortable or loose-fitting clothing to your appointment.
“Many patients don’t realize this, but most of your clothing can be left on for spinal injections,” adds Dr. Mizrahi. “This is a nice added comfort level, leaving pants, socks and even shoes on. We will expose the area we are working in just enough to safely perform the procedure.”
- Lay face down on the procedural table.
The procedure itself can take anywhere from 10 to 20 minutes, depending on your needs. If you are anxious about the procedure, mild sedation may be an option – talk to your doctor in advance if you have any worries or concerns.
“A lot of patients think they’ll need twilight or to be put under anesthesia for this kind of injection, but I rarely use any kind of sedation,” explains Dr. Mizrahi. “Communication throughout the procedure helps to calm patients down. I even like to play music in the room – it makes everyone feel a bit more comfortable.”
- Your back will be cleaned and sterilized before the injection.
- You’ll feel a slight pinch when the needle is placed.
Your physician may use a local anesthetic to numb the area, but it may not be necessary if very thin needles are used.
- X-ray guidance will help determine the exact placement of the needle.
“When we do these types of injections, we use fluoroscopic (x-ray) guidance to make sure the needle is going exactly where it needs to,” says Dr. Mizrahi.
Multiple images are taken both before needle placement and each time the needle is adjusted. “Because x-ray is a 2-dimensional image, we change the position of the x-ray often to gauge depth, and get a 3D understanding of where the needle tip is,” he adds.
- Contrast will be injected.
“The number one, most important thing is to make sure the needle is not somewhere where an injection could be harmful,” Dr. Mizrahi explains.
Contrast dye is used to verify needle positioning. The dye will show up as gray or black on XRAY and will show the flow of medication to be injected, ensuring it is the desired location, is likely to help your pain, and not somewhere potentially harmful such as in a blood vessel.
- Once the needle is confirmed to be in the correct location, the medication is injected.
For an epidural spinal injection, the solution is a combination of:- Numbing medication: numbs the nerve to reduce pain
- Steroid: helps to reduce inflammation
- Saline: increases the volume of the solution, and washes away pain and inflammatory chemicals in the area
“Some patients may feel a slight worsening of their usual pain, ex: sciatica down the leg before the medication kicks in,” says Dr. Mizrahi. “Because we’re adding medication to an already tight or irritated area, there could be a slight flare-up, but flare-ups are not common, usually short-lived, and tolerable.”
- The needle is removed and the area is cleaned and covered with a bandaid.
- Vitals are taken one last time, and you can head home.
When will the injection kick in, and start working? And how long can relief last?
“Patients may start feeling relief as early as the day of the injection, but the steroid peaks around 7 to 10 days afterward,” says Dr. Mizrahi.
Pain relief will vary from patient to patient, but Dr. Mizrahi shares that his goal is for at least50% improvement in pain and function for 3 months. “Sometimes it lasts longer, other times it doesn’t — the results are all a function of how bad someone’s underlying problem is,” he says.
What Injections Don’t Do:
Epidural injections for back pain can provide relief, but they don’t fix the underlying issue that is causing your back pain. The only way to “fix” the problem is likely surgery but that is necessary less often than most think.
“If you’re feeling better after injections, and you’re not necessarily ready or a candidate for surgery, that’s okay! Injections can provide much-needed relief. If your pain is better, you can exercise and function as normal, then there’s no need to rush towards surgery,” Dr. Mizrahi shares.
When should you consider injections?
If you’re suffering from chronic back pain, you should:
- Be evaluated by a professional. A pain management specialist, physical therapist or spine surgeon should assess your situation to help determine the root cause of pain.
- Try conservative options first. Your doctor should prescribe physical therapy and/or medications to manage the pain and see if that makes a meaningful difference.
- If not, consider injections. If conservative management fails, there are many different types of procedures that may help but should be specifically tailored to your individual diagnosis.
- Get multiple opinions. “Especially before having any surgery, get multiple opinions. While this can be time-consuming, you want to be as thorough as possible,” advises Dr. Mizrahi.
If you’re scared of needles or have concerns about pain management injections, Dr. Mizrahi assuages our fears, sharing, “After having injections, 90% of my patients say it was a lot better than they thought it would be.”
Next Steps & Resources:
- Meet our sources: Mike Mizrahi, D.O.
- To make an appointment with a pain management specialist near you, call 800-822-8905 or visit our website.
- Learn more about pain management services at Hackensack Meridian Health.
Find a doctor near me
What’s the Source of Your Back Pain?
Answers to 10 Common Questions About Back Pain

6 Tips for Back Pain Arthritis Relief
